Digital Obesity Care Reaches Socioeconomically Diverse Patients
In a real-world cohort of over 40,000 people living with obesity, digital care engaged patients across all socioeconomic groups, including low- and middle-income populations. However, affordability emerged as the primary driver of treatment discontinuation, with economic barriers disproportionately limiting long-term access and continuity of care.


Occupational Distribution in a Real-World Digital Care Population (PO4.209)
Anna Sommerfeld1, Kristofer Ringner1, Elin Skoglund1, Oliver Willacy1, Felix Wittström1, David Buchebner1, Martin Carlsson1,2
1. Yazen Health AB, Malmö, Sweden
2. Department of Medicine and Optometry, eHealth Institute, Linnaeus University, Kalmar, Sweden
INTRODUCTION
Obesity disproportionately affects individuals from lower socioeconomic backgrounds, with obesity prevalence estimated to be 70–80% higher in low- compared with high-income adults in Sweden. Access to effective obesity treatment remains uneven across socioeconomic groups, and novel pharmacological therapies are costly and not reimbursed, requiring patients to bear the full cost themselves, which may further widen existing health inequalities in long-term treatment outcomes. While digital care models may improve access and continuity of care, the socioeconomic and occupational profiles of patients treated within digital obesity care remain insufficiently explored.
METHODS
The study population comprised 40,254 Swedish adults living with obesity (mean initial BMI 33.4 kg/m²; mean age 49 years; 70% women) receiving care at Yazen Health, a licensed private Swedish healthcare provider offering a multidisciplinary digital obesity care model for people with obesity.
Occupational data were used as a proxy for socioeconomic status and classified according to the Swedish Standard Classification of Occupations (SSYK 2012) and ISCO-08 major groups. Patients were categorised into low-, middle-, or high-income groups; individual income data were not available. Formal SSYK-based classifications were retained for income grouping and health economic analyses. Self-reported reasons for treatment discontinuation were analysed descriptively. Managers within healthcare were classified as healthcare professionals to reflect healthcare training and domain expertise, while managers in other occupational groups were classified by managerial function.

RESULTS
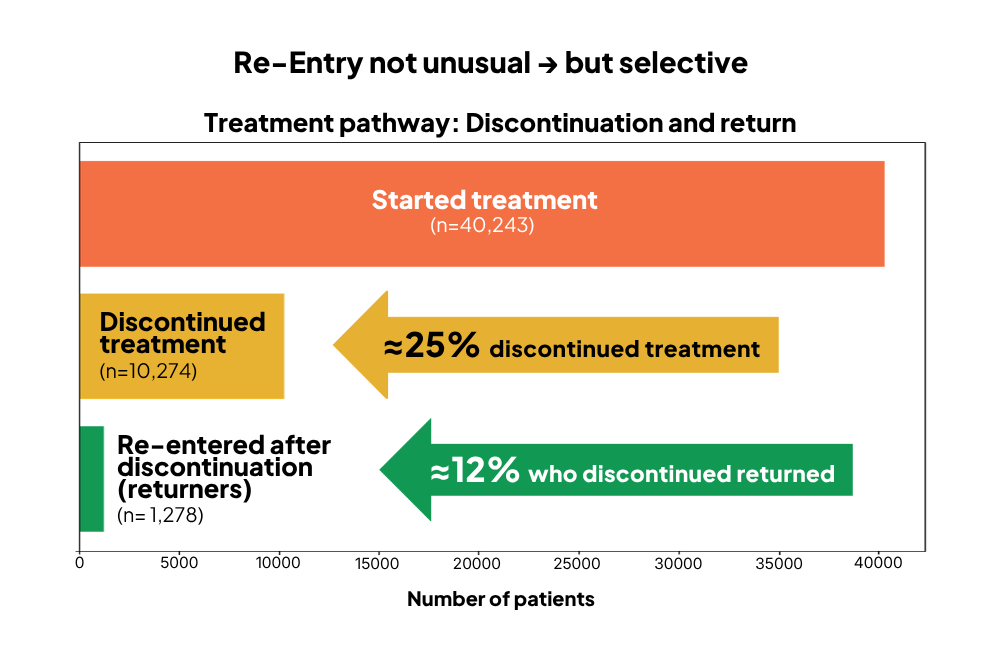
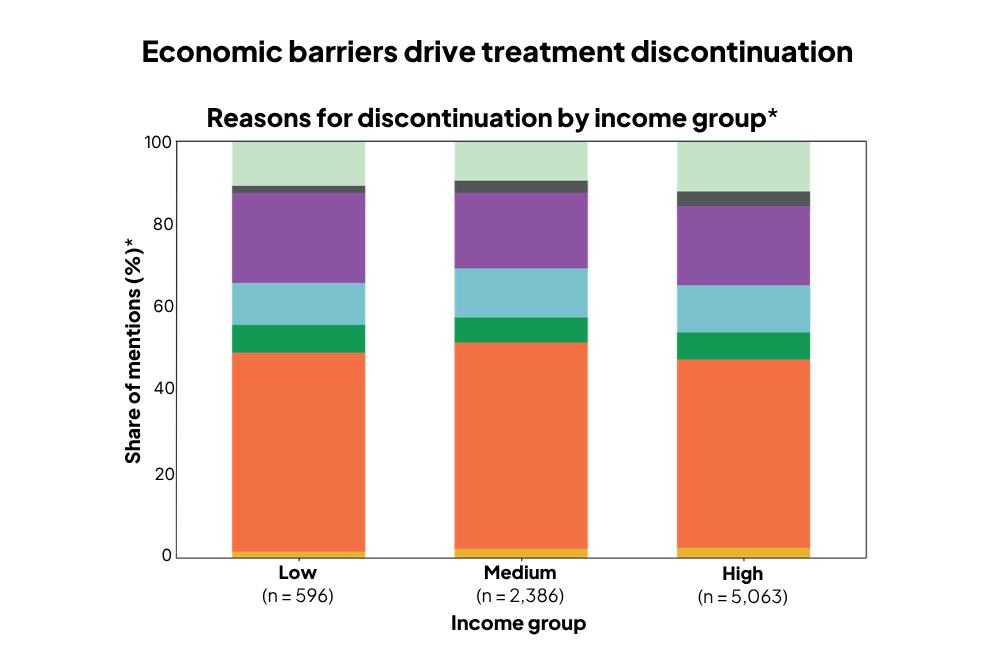
Based on occupation-derived socioeconomic grouping, 35% of patients were classified as low-income, 38% as middle-income, and 27% as high-income, compared with approximately 12%, 80%, and 8% in the general Swedish population, respectively, according to income-based economic standard (Statistics Sweden, SCB). Healthcare professionals constituted the largest occupational group (21.8%), with nurses and nurse assistants accounting for 72.5% of this group (15.9% of the total population), representing predominantly lower- to middle-income occupations. Approximately 25% of patients discontinued treatment, and 12.4% subsequently re-entered care. Economic reasons were the most frequently reported cause of discontinuation (40.9%). Return to treatment was most common among high-income individuals (61.6%), whereas discontinuation was more often permanent among low- and middle-income patients, with only 8.2% and 30.7% returning, respectively.


.webp)
CONCLUSION
Digital obesity care models can engage socioeconomically diverse and traditionally underserved populations, even within entirely self-funded care settings. However, affordability emerges as a key determinant of sustained access to obesity care, with economic barriers disproportionately limiting long-term treatment continuity among lower-income patients.
Digital care can reach socioeconomically diverse populations.
Affordability is a key determinant of long-term access.
Findings support the need for:
- Reimbursement
- Targeted financial support
- Equity-Focused Obesity Policies
References:

May 11, 2026
May 12, 2026
Start your weight loss journey with Yazen today
Everything you need to do is to create an account and answer some questions about your health
.svg)
.svg)
More articles
The Yazen Model - Modern Obesity Treatment Given Via a Digital Care Model. A Descriptive Analysis
The Yazen Model enables modern obesity treatment, integrating medical treatment, lifestyle intervention and social support. By now*, more than 30,000 patients have received treatment using this model.
Summary
The Yazen Model goes beyond traditional methods, providing patients with the tools to manage their disease, addressing medical and behavioural aspects, education and social support via a digital platform for accessible, continuous and effective weight loss and management.
High-Volume Patient–Caregiver Interactions in a Fully Digital Obesity Care Model
This real-world analysis quantifies patient–caregiver interactions in a fully digital obesity care model with unlimited follow-up.
Summary
Across 156 weeks, 7.7 million messages were exchanged between 50.414 patients and a multidisciplinary team (mean 5.5 per patient/week), and 2.3 million weight entries were logged, highlighting how a fully digital care pathway enables continuous patient engagement and sustained self-monitoring over time.



.svg)

.webp)


.webp)